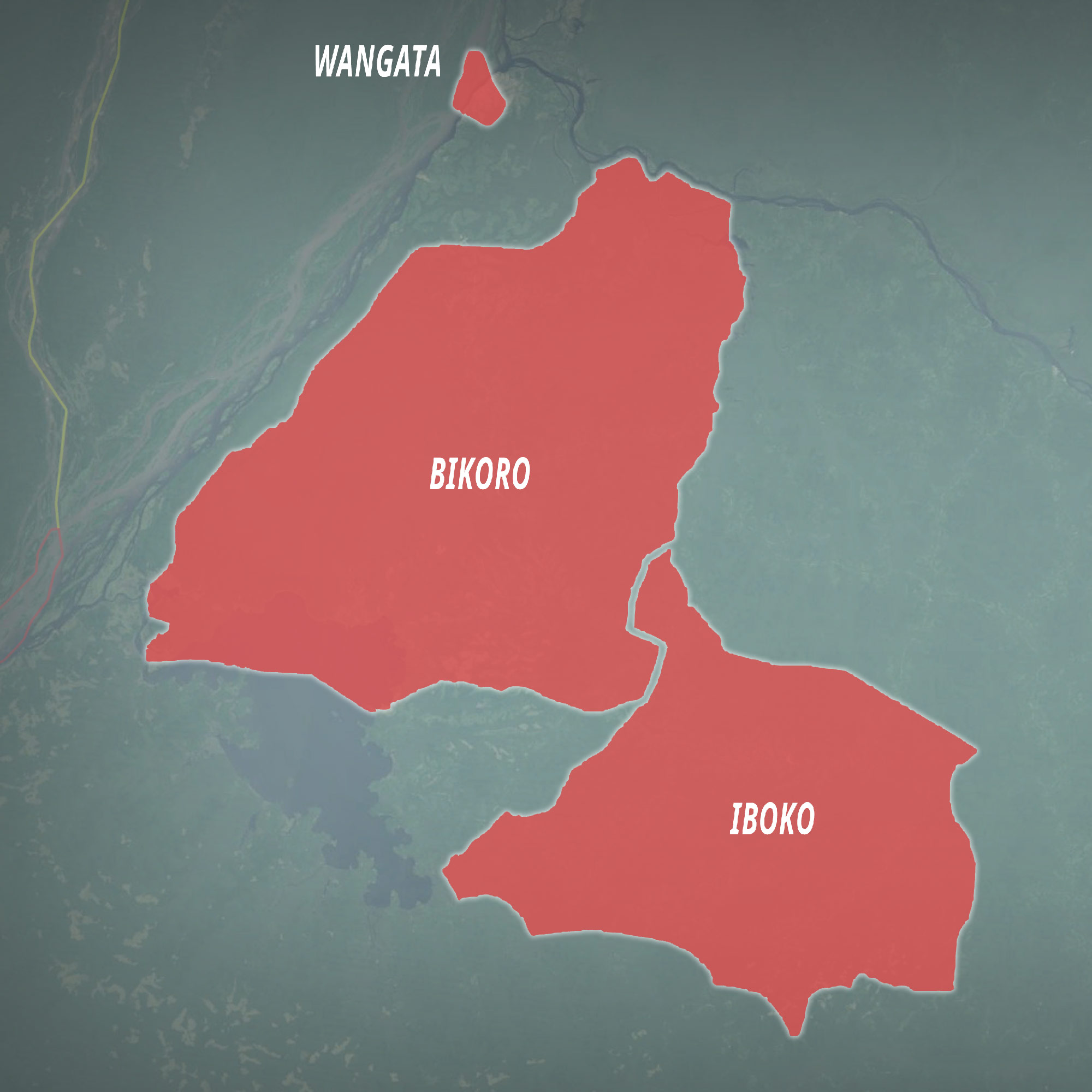
The Ebola outbreak in the Democratic Republic of the Congo appears to be in its waning days. Despite 28 deaths as of early June, health officials are cautiously optimistic that they are bringing the outbreak under control. So far, it’s a striking turnaround from the 2014 West Africa outbreak, which killed more than 11,000 people in Liberia, Sierra Leone and Guinea, and traveled as far as Glasgow, Scotland, and Dallas, Texas.
Despite difficult-to-traverse terrain and local communities’ skepticism of health care workers, from the start of the outbreak, officials got in front of the disease and kept it in check. Several factors made the DRC response markedly different than previous outbreaks, saving countless lives.
1. Long distances between villages and an underdeveloped infrastructure slowed the spread of the disease.
The DRC’s remoteness made it difficult for health care workers to access affected communities, but it also impeded the spread of the disease. For the most part, infected individuals did not leave their communities, and outsiders didn’t come in, greatly limiting the number of infections. In contrast, in 2014, at the height of the West Africa epidemic, Ebola spread quickly through densely populated cities.
“The risk zero doesn’t exist. That is what we need to have all in mind. The risk for the virus to escape to neighboring countries is there. But with the actions — the strong actions that the government is taking now — it can limit the spread of this disease, first of all in the Congo itself, and in neighboring countries.”

Djoudalbaye BenjaminHead of Policy and Health Diplomacy, Africa Centres for Disease Control and Prevention